Hip Abductor Weakness
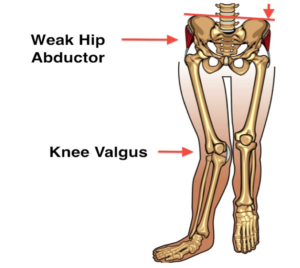
The main job of your hip muscles is to maintain proper alignment of your leg when you move. One of the primary hip muscles, the gluteus medius, plays an especially important stabilizing role when you walk, run, or squat. The gluteus medius connects your thigh bone to the crest of your hip.
When you lift your left leg, your right gluteus medius must contract to keep your body from tipping toward the left. And when you’re standing on a bent leg, the gluteus medius helps prevent that knee from collapsing inward into a “knock knee” or “valgus” position.
Here is a video showing hip abductor weakness in action.
This weakness is also a contributing factor to Lower Cross Syndrome.
Hip abductor muscle weakness (gluteus medius) lets your pelvis drop and your knee dive inward while walking or running. This creates significant strain on the hip and knee and can lead to a cascade of other issues.
When the knee dives inward, it pushes the kneecap outward, causing it to rub harder against the thigh bone—resulting in irritation and, over time, arthritis. Walking or running with a “knock knee” posture also places extreme stress on the ligaments around your knee, making sprains more likely.
Downstream and Upstream Impact
Hip abductor weakness is seen more frequently in females, especially athletic individuals.
What to Avoid If You Have Hip Abductor Weakness
You may benefit from arch supports or custom orthotics if you have fallen arches.
If you are overweight, reducing body weight can decrease stress on the hip muscles and improve outcomes.
Why Strength Training Matters
The most important treatment for hip abductor weakness is strength training.
Building strength in the hip muscles is directly tied to symptom relief. In fact, individuals with stronger hips are far less likely to experience injuries in the first place.
The exercises listed below are critical for your recovery.
Tools We Use to Help Correct Hip Abductor Weakness
Myofascial Release
Overworked muscles often become tight and develop knots or “trigger points.” Chronic tightness leads to inflammation and swelling, eventually creating adhesions between tissues.
Your chiropractor may use hands-on techniques or specialized tools to release these tight areas and break up adhesions. This process improves circulation, relieves pain, and restores flexibility.
Therapeutic Exercise
Muscle tightness or weakness interferes with joint function and causes discomfort. Through specific stretching and strengthening techniques, your chiropractor will target the right muscles to improve flexibility, build strength, and ease pain.
Healthy, strong, and flexible muscles help prevent re-injury and support long-term joint health.
How We Use Multiple Therapies to Help You Rebuild Stability
At Ashworth Chiropractic in West Des Moines, we understand that hip abductor weakness doesn’t always respond to a single approach.
That’s why we combine four complementary services—chiropractic care, massage therapy, acupuncture, and physical therapy—to help you regain strength, improve movement, and reduce your risk of setbacks.
Here’s how each one contributes something different to your recovery.
Chiropractic Care: Reinforce Pelvic and Spinal Alignment
Our chiropractors assess how your spine and pelvis may be affecting overall muscle performance.
Gentle adjustments support better coordination between joints and muscles, making it easier for your body to move efficiently during your recovery program.
Massage Therapy: Support Recovery After Activity
As you begin strengthening weak hip muscles, other areas may become sore or overworked.
Massage therapy helps reduce post-exercise soreness, ease soft tissue fatigue, and support faster recovery—especially helpful if tightness or discomfort is slowing your progress.
Acupuncture: Calm Overactive Muscles and Nerves
Chronic tension or nerve sensitivity can limit how well the hips respond to treatment.
Acupuncture helps by improving blood flow to hard-to-reach areas, calming overactive nerves, and creating a better internal environment for healing.
Physical Therapy: Customize and Progress Your Rehab
Beyond general exercise, our physical therapists build targeted programs to match your stage of recovery—from early activation to advanced stability.
This personalized guidance ensures you’re strengthening the right muscles, the right way, at the right pace.
One Coordinated Plan, Built for Long-Term Relief
Together, these services allow us to build a treatment plan that’s not only tailored—but also adaptable.
Whether you’re struggling with instability, pain, or progress plateaus, we’re here to guide you forward with a collaborative care model designed around your goals.